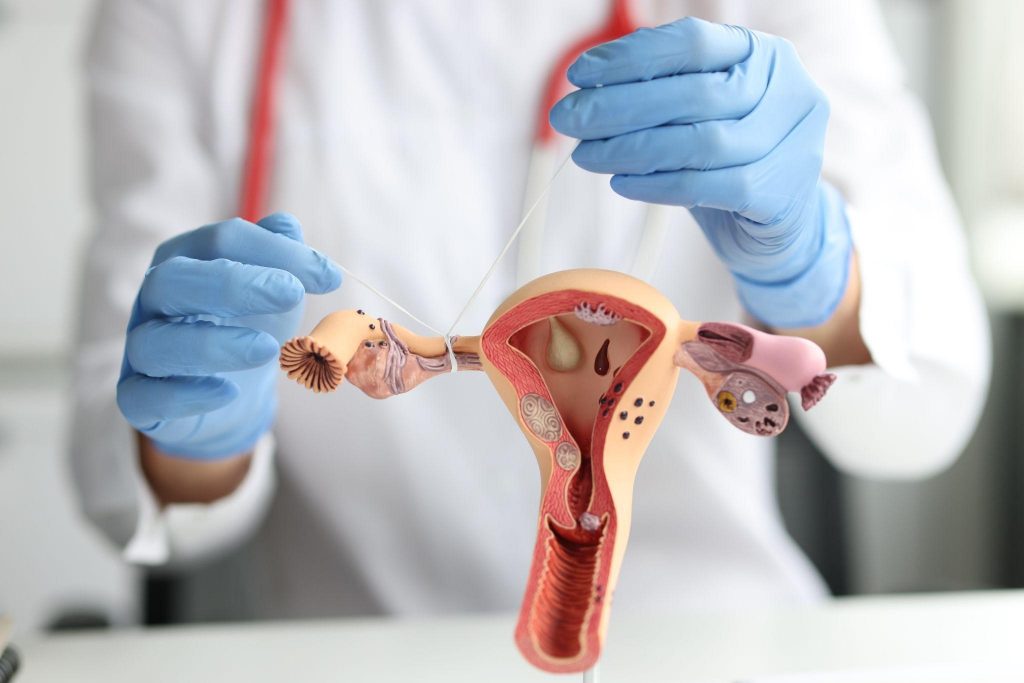
Causes of Blocked Fallopian Tubes

Blocked fallopian tubes are a common cause of female infertility, preventing the egg from traveling down the tube to meet the sperm and be fertilized. Various factors and conditions can lead to this issue: Pelvic Inflammatory Disease Pelvic Inflammatory Disease (PID): This infection of the reproductive organs can cause scarring or damage to the fallopian […]
Breakthrough Therapy: Opening Blocked Fallopian Tubes Without Surgery

Introduction: In a remarkable breakthrough, scientists have unveiled a groundbreaking therapy that has the potential to open completely blocked fallopian tubes, offering new hope to women struggling with infertility. Presented at the Annual Meeting of the American Society for Reproductive Medicine (ASRM), this therapy, which resembles a deep infertility massage, could revolutionize the treatment landscape […]
You Have Blocked Fallopian Tubes, Do You Need Surgery to Remove Them?

You were just diagnosed with blocked fallopian tubes or fallopian tubes that are swollen and clogged with fluid which is called hydrosalpinx. Your OB-GYN says you can have surgery to open the tubes which is called a Salpingostomy (also called neosalpingostomy) but the documented rates of pregnancy after a salpingostomy is not stellar…pregnancy rates after […]
Effective Nonsurgical Treatment for Blocked Fallopian Tubes?
Unlock the potential for natural conception with Clear Passage’s groundbreaking, non-surgical therapy that has successfully opened blocked fallopian tubes for 61% of women, offering hope and a 57% pregnancy rate without the risks of surgery. Contact us today for a Free Consult or to Request Information. To learn more visit our Apply to Therapy page. […]
Opening Blocked Fallopian Tubes

Comparing Treatment Options PROCEDURE PREGNANCY RATE COSTS Clear Passage® Bodywork 39.33% ii $6,500 In Vitro fertilization (IVF) 30.87% iii $15,000 – $30,000 iv IVF after Clear Passage 56.16% ii, iii $21,500 – $36,500 iv What Is Clear Passage? What Occurs in Therapy? Over 1,000 Babies Born Treatment Options Explained What are Blocked Tubes? Symptoms of […]
Blocked Fallopian Tubes

APPLY FOR FERTILITY LOAN Opening Blocked Fallopian Tubes – Naturally Unlocking the Path to Pregnancy A Natural Treatment for Blocked Fallopian Tubes Discover our natural approach to open tubal blockages and enhance fertility without surgery. Clear Passage®️, a pioneer with three decades of experience, has successfully restored function to hundreds of totally blocked tubes, including […]
Patient Story – Blocked Fallopian Tubes
Surgically “Unopenable” Fallopian Tubes Autumn’s Story Six years ago my partner and I made the decision to start trying to have a baby. She already had a son she had conceived through artificial insemination, and he was two years old at the time. I had always wanted children and thought it would be an easy […]
7 Myths About Blocked Fallopian Tubes

1. “Just relax, it will happen.” This myth is a crowd favorite and probably one of the most frustrating, often perpetuated by those who have not personally dealt with infertility. You may have been subjected to the knee-jerk statement “Just stop trying so hard.” Wouldn’t it be great if you could clear your fallopian tubes by […]
Patient Story: Two Natural Pregnancies After Blocked Fallopian Tubes

apply for therapy patient stories Julie, a former patient, talks about treatment at Clear Passage and how it has changed her life. What brought you to Clear Passage? I had an IUD put in in 2009. Immediately afterward, I began to experience a little pain during intercourse which got worse until I got the IUD […]
Study Shows Alternative Therapy for Infertility Opens Blocked Fallopian Tubes Without Surgery

Endorsed by gynecologists, Clear Passage Physical Therapy® treats infertility using all-natural, hands-only approach GAINESVILLE, FL – Developed by a group of leading physicians, including research gynecologist and former Chief of Staff of North Florida Regional Medical Center, Richard King, M.D, Clear Passage Physical Therapy’s all-natural holistic infertility massage to the reproductive organs opens blocked fallopian […]