Overview
Pain at the tailbone (coccyx bone) can range from inconvenient to totally debilitating. As pain increases, some people find it difficult or virtually impossible to sit – making their lives miserable. Unfortunately, very few treatment regimens have been studied to treat this condition.
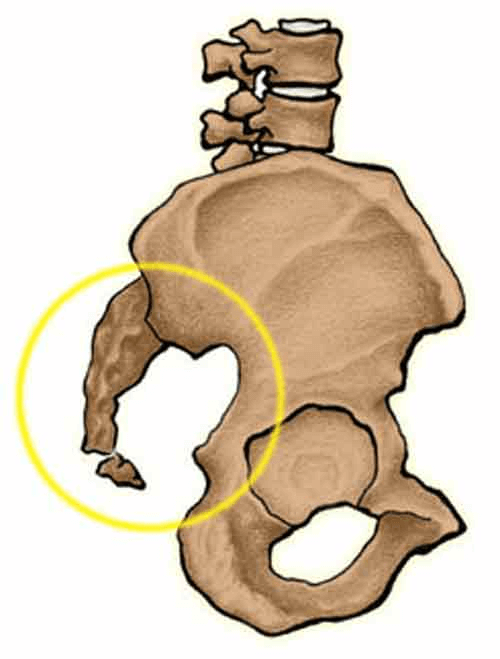
Coccyx pain (coccydynia or coccygodynia) generally begins with a trauma – often a fall or accident that pushes the tailbone forward or to the side. Persistent or repeated pressures on the xoxxyx from horseback riding, bicycling or similar seating sports, or even office sitting for long hours can cause tailbone pain. It can also occur after a pelvic surgery or infection.
As the body begins to heal, strong collagen fibers, similar to the strands of a nylon rope, lay down in a random pattern across the injured area. These fibers attach to the traumatized tissues and to each other with a chemical-molecular bond in a process called cross-linking. As they lay down one upon the other, they create adhesions (internal scars) to help stop bleeding and to isolate the injury, as the first step in healing.
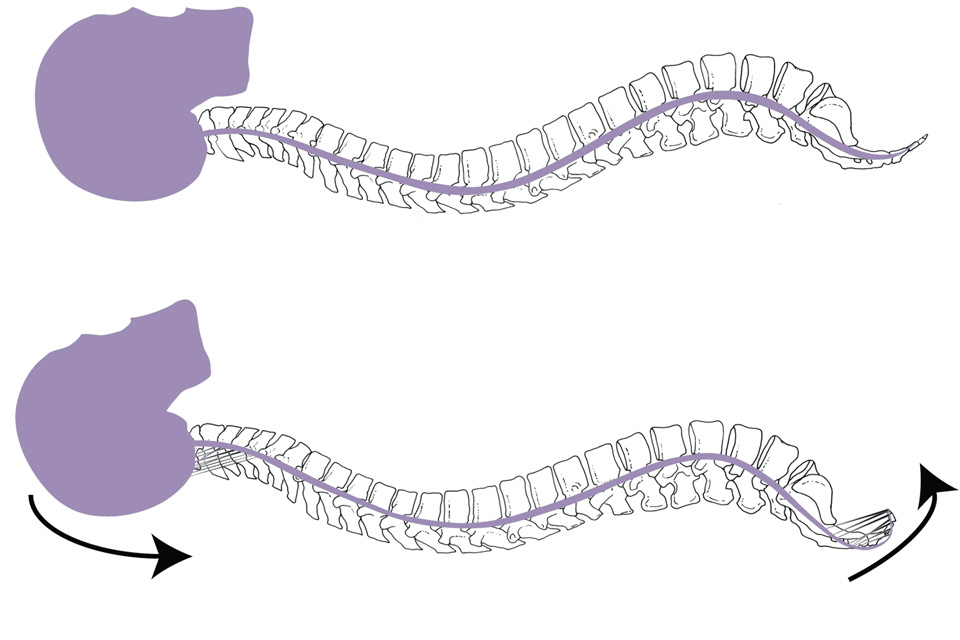
Once the body has healed, these linked fibers remain in place. The resulting bond can leave the tailbone stuck in a position that is forward, bent to the side or both. This flexed position of the tailbone can cause inflammation that is exacerbated with sitting. Unable to move out of the way when a person has a bowel movement or a woman has intercourse, the fixed position of the tailbone can act like a partially closed door, causing significant pain with these movements. Sometimes the tailbone sticks out at an unnatural angle causing pain while sitting.
Physicians will sometimes suggest an anti-inflammatory or may inject a steroid along with a numbing agent, to help decrease the pain. These can provide temporary relief in some cases. Since these treatments focus more on the symptom than the cause of the pain, they may not provide a long-term solution.
Avoiding Surgery (Coccygectomy)
When pain is persistent or severe, patients begin to seek other treatments for their tailbone pain in order to regain quality of life. Some become so frustrated that they opt to have part or all of the tailbone surgically removed. While we have seen this help in some cases, for other patients surgery has brought a lifetime of constant, debilitating pain – often worse than the original tailbone pain.
The intent of surgery is generally to remove the coccyx so it no longer causes pain. The intent of therapy, on the other hand, is to free the bound tissues, enabling the coccyx to return to normal – to the usual pain-free position and flexibility it had before the trauma and healing events occurred.
Discover lasting relief from tailbone pain without surgery – Clear Passage Physical Therapy offers a Free Consultation and Request Info to explore their unique, non-invasive approach that has helped countless patients regain comfort and mobility, potentially avoiding risky coccygectomy and its long, painful recovery. To learn more visit our Apply to Therapy page.
Two Forms of Treatment
According to medical literature, adhesions in the abdomen or pelvis can be addressed in two distinctly different ways:
- Clear Passage®️ Approach
- Surgery (coccygectomy)
Therapy to Decrease Adhesions
Description of the procedure. The Clear Passage®️ Approach is a manual physical therapy that uses no drugs and no surgery. It has been cited in numerous studies and peer-reviewed medical journals for its ability to decrease adhesions. The studies show effectiveness with abdominopelvic pain and dysfunction caused by adhesions.
In the case of coccydynia (tailbone pain or coccyx pain), we find the tailbone is generally bound by adhesions that formed after the initial trauma or cause. In these cases, the coccyx may be pulled forward or to the side (or both), causing inflammation and pain. The pain often increases with movements such as sitting, bowel movements and sexual intercourse.
To relieve the pain and return the body to pain-free mobility and function, we focus on decreasing the adhesions pulling the coccyx out of its normal position. We start with a thorough evaluation of the entire body, with a focus on the structures of the pelvis and lower back. We want to bring all of those areas into symmetry. We suggest – but do not require – that a person with coccyx pain undergo internal treatment via a gloved finger in the vagina or rectum. Due to the structure of the coccyx and its supporting ligaments, success may be limited without internal treatment. We always discuss the need for internal treatment with the patient before starting, and show the utmost respect for the patient’s privacy and comfort.
A good analogy to this part of the treatment is a pup tent, with poles at the front and back held in midline position by ropes on each side. If the rope on one side is pulled too tight, the pole will bend to the side, forward or backward in a strained, awkward position. By loosening the tightness and restrictions, we return to the normal symmetry and tone – with easy, equal pressure on each side.
This therapy is ‘all natural’ in that it is 100 % ‘hands-on.’ Patients describe it as feeling like a very deep massage. In some areas, the therapy can sometimes be much lighter, depending on the area and depth being treated. Internal treatment is often described as feeling like pressure, rather than pain.
We use our hands to find adhered areas. We work to deform and detach the tiny strands that comprise adhesions – similar to pulling out the strands of a nylon rope or pulling out the run in a sweater. Your therapist may describe it as “pulling out salt-water taffy, in very slow motion.”
The therapy is site-specific; our therapists are experts at palpating and manipulating the soft tissues of the body – where adhesions generally form. We use data from the patient’s history, direct feedback from the patient during therapy, and a thorough training and understanding of methods developed over 30 years to deform and detach the molecular/chemical bonds that are at the core of adhesions. The usual protocol, which is cited in our studies, consists of 20 hours of therapy spaced over five days. Treatment for coccyx pain can generally be completed in as little as 10 hours. A small percentage of the work, generally around 10 to 15 percent, is performed internally. View a short video of what Clear Passage®️ therapy feels like.
Advantages of Therapy
Direct access to the adhesions that are causing the pain. Due to its location and accessibility, we can directly palpate and treat adhesions that are pulling the coccyx out of its normally relaxed, midline position. In doing so, we do not cut or burn anything in your body; we do not remove anything from your body. Our focus is to deform and detach adhesions.
No hospitalization. Therapy is performed in a private treatment room, one-on-one with a highly skilled therapist certified in the work. Patients may bring a partner or family member along for company, if they like.
No anesthesia. The patient is awake and communicative during therapy. Patient involvement is encouraged, with the patient invited to give feedback throughout the course of therapy.
Decreased risk. Risk is minimal. There is no cutting or burning, and no risk of side effects from anesthesia or medications.
No foreign bodies are introduced. No staples, stitches, films, meshes or surgical instruments are inserted into the body.
Side effects are mild and transient. The most common side effects reported with therapy are temporary tenderness, aching, fatigue and hip or back pain. When they occur, these symptoms pass within a few days.
Improvements in other areas of the body. Because therapy focuses on detaching adhesions throughout the body, with a particular focus on the pelvis and the low back for tailbone patients, patients regularly report significant increases in flexibility and range of motion after therapy. Many report decreased pain and/or increased function in areas near the site where they are being treated. Some report this in areas where they had forgotten or had not realized they were having a problem, until therapy relieved the pain or tightness. A significant number report decreased back, neck and headache pain due to relieving pressure on the spinal cord up to the base of the skull.
Written reports. After therapy, we send each patient a typed, detailed Initial Evaluation along with a typed Progress Report or Discharge Summary. If needed, we are glad to send you daily notes of every therapy session.
Disadvantages: Risks and Challenges of Therapy
Temporary soreness. Some people report temporary soreness during therapy, which dissipates within a few days.
Costs of therapy are generally a fraction of the cost of surgery; as with surgery, insurance reimbursement may vary based on your insurer and your plan. Clear Passage®️ is an out-of-network provider for your insurer.
Travel and time are a consideration. The 20 hour therapy protocol generally takes five days (e.g., Monday – Friday);a 10 hour session takes half as long (figure 2 1/2 days).Our therapy is only provided by trained, certified therapists in several cities in the U.S. and U.K, and designed for out-of-town and out-of-country patients. Most patients fly to the clinic city during the weekend, start therapy Monday morning and are done before the next weekend.
Surgery to Remove Part or All of the Coccyx
Description of common procedures. The surgical option, coccygectomy to remove part or all of the tailbone, is rarely performed. Recovery can be long and uncomfortable for the patient. In general, the surgery involves creating a one to two-inch incision over the top of the coccyx. The bone covering (periosteum) is then dissected away from the bone. This allows the coccyx to be separated from the sacrum.
Unless complications arise, the operation is brief and may be done on an outpatient basis. The most difficult part of the operation is the long time it takes for the patient to heal. Reports show that it may take three months or longer after the surgery before patients note the desired relief from their symptoms. Naturally, sitting is very difficult throughout the healing process.
iew surgery to remove part of a coccyx by clicking here.
Advantages of Surgery
Ease of access. The surgeon can easily access the coccyx and surgical removal is relatively easy, in most cases.
Disadvantages: Surgical Risks and Challenges
Long, painful recovery. As noted above, recovery from coccyx bone removal (coccygectomy) has been documented take up to a year. Because the area is involved with basic daily activities (sitting, bowel movements, sexual intercourse), the recovery time can linger since the remaining portion of the sacrum cannot be isolated without activity in order to heal quickly.
Uncertain outcomes. In some cases we have seen, surgery to remove the tailbone has been very successful. In other cases, it has brought a lifetime of pain – more debilitating than the pain before surgery.
Hospitalization during recovery. In some cases, patients must undergo a hospital stay after surgery to remove the coccyx. Patients are monitored to ensure their recovery and that there are no immediate post-surgical complications or infections.
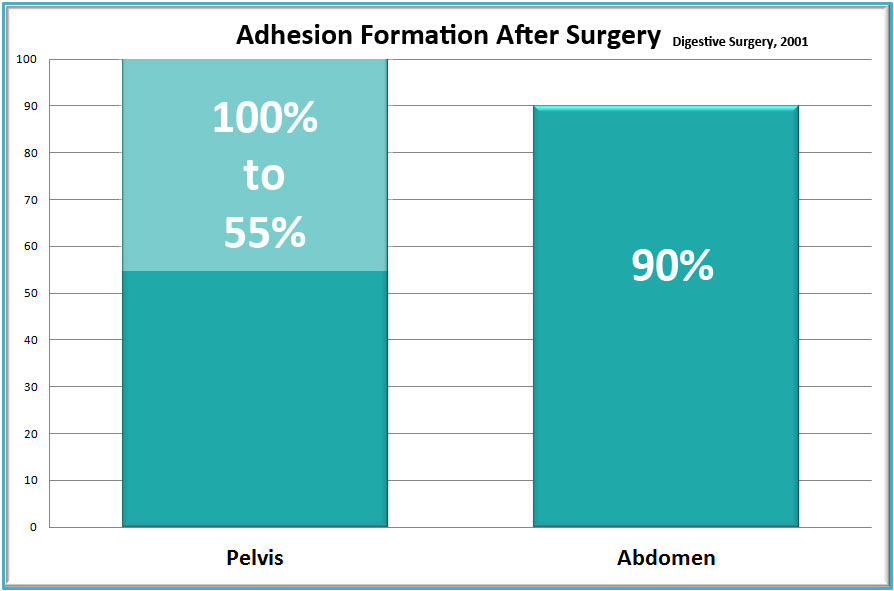
New adhesions generally form after surgery. Medical literature compiled from over 50 years of abdominal and pelvic surgeries shows that nearly all surgeries cause new adhesions to form. Thus, despite the skills of the finest surgeon, adhesions often recur, sometimes worse than before surgery. Because surgeries cause adhesions, some or our patients feel trapped in a cycle of pain-surgery-adhesions, with no end in sight.
Pre-Treatment Screening (Surgery and Therapy)
Both therapy and surgery require patients to be screened for appropriateness and contraindications before treatment.
Screening before therapy. Before therapy, Clear Passage®️ directors consult applicants to review goals, risks and potential benefits they can expect. We conduct a thorough review of the applicant’s history of healing events (prior surgery, trauma, infection, endometriosis, etc.) to determine if and where adhesions have likely formed and how they might be causing problems.
We screen applicants for two reasons:
- to determine the likelihood that we can help an applicant reach his/her goal, and
- to rule out contraindications which could decrease effectiveness of therapy or cause problems.
Screening before surgery. Before surgery, physicians consult patients to review the goals, risks and potential rewards they can expect from the procedure. They may order diagnostic tests to help rule out contraindications, such as active infection, and to help identify problem areas in the body that should be assessed during surgery. It is reasonable to ask your doctor about the likelihood of adhesion formation after surgery.
Related Content:
Avoid Surgeries: Adhesions | Blocked Fallopian Tubes | Endometriosis | PCOS | SBO | Surgery Risks | Tailbone